Ocular Allergy
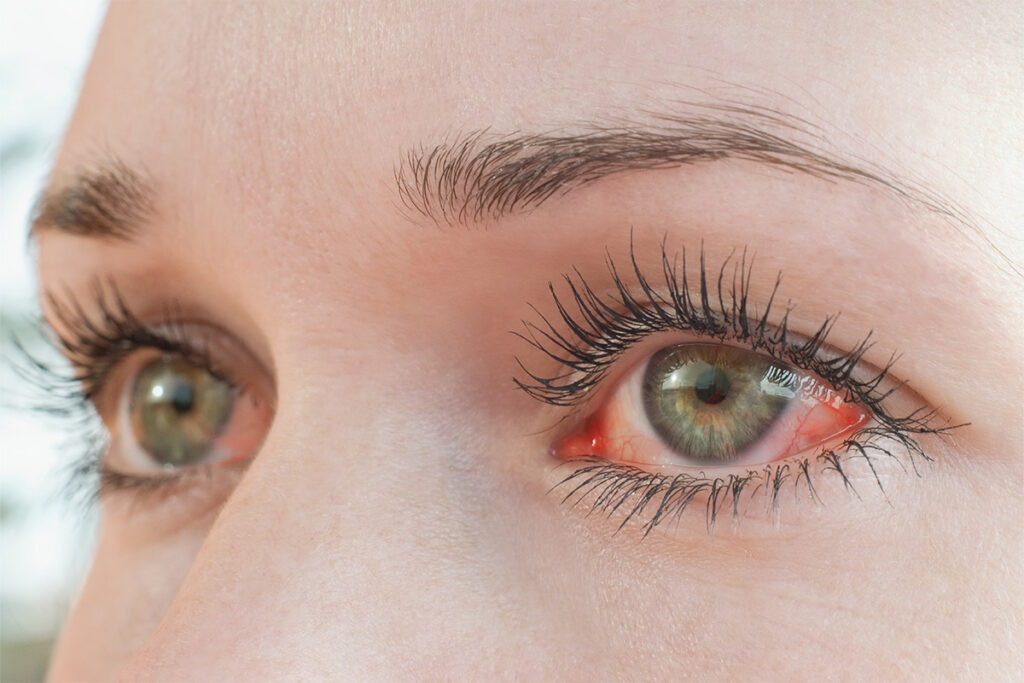
What is ocular allergy?
Ocular allergy is an inflammatory reaction of the surface of the eye to particles (allergens) in the environment. It is quite common and affects people of all ages. Inflammation can be asymptomatic, or cause dramatic symptoms, and in severe cases, severe loss of vision.
What are different types of ocular allergy?
There are five types of ocular allergy.
- Seasonal allergic conjunctivitis, or hay fever conjunctivitis, occurs during certain seasons when environmental allergens are more plentiful.
- Perennial allergic conjunctivitis is similar, but is year long.
- Giant papillary conjunctivitis (GPC) is the result of particles that adhere to contact lenses that cause large mounds of inflammatory cells to accumulate under the inner eyelid surface.
- Vernal keratoconjunctivitis (VKC) is a severe form, usually occurring in younger patients in warm climates, which often causes thick, stringy mucous secretions and severe redness and itching.
- Atopic keratoconjunctivitis (AKC) is also severe, with pronounced allergic symptoms, and is associated with systemic allergy and atopy. The last two are potentially blinding diseases.
What causes ocular allergy?
Exposure of susceptible individuals to allergens such as pollen, ragweed, or pet dander may allow these particles to bind to special antibody receptors that then trigger a cascade of inflammatory events involving the release of histamine and the activation of inflammatory cells called mast cells, and at times eosinophils.
Particles which adhere to contact lenses or even some topical eye drops can also be triggers. Histamine causes blood vessels to leak fluid, protein, and inflammatory cells into the area of exposure, causing many of the symptoms of allergy.
Inflammatory cells can further propagate the response, and in severe ocular allergy such as VKC or AKC, can release enzymes that damage the cornea leading to growth of new blood vessels, scarring, and permanent loss of vision.
What are the symptoms of ocular allergy?
- Redness
- Itching
- Light sensitivity
- Tearing
- Burning
- Eyelid swelling
- Swelling of the conjunctiva
- Decrease in vision
- Runny nose or sneezing
As above, sometimes ocular allergy can be asymptomatic, or more likely unrealized, finally seen on examination by the ophthalmologist.
What other medical conditions are associated with ocular allergy?
Ocular allergy can occur on its own, but typically occurs in conjunction with allergic rhinitis or sinusitis. It is not uncommon to see those who suffer from allergy to have other systemic diseases such as eczema or asthma, especially in AKC.
How is ocular allergy diagnosed?
Redness and other symptoms which occur along with seasonal allergies or at certain times of year also suggest allergy.
Review of medical history for eczema and asthma, and a family history for allergic disease, are also important.
Response of symptoms to anti-allergy medication may help indicate whether allergy is involved.
Allergy testing and review of the patient’s life from top to bottom may reveal possible sources, some which have been around for years and unknown to the patient to be driving inflammation.
Slit lamp examination often reveals characteristic bumps on conjunctiva, especially underneath the upper and lower eyelids, which correspond to swelling and collections of inflammatory cells.
Rarely, severe cases may show spread of new blood vessels toward the middle of the cornea, usually irreversible, or worse still, scarring and growth of conjunctiva over the entire cornea leading to near complete loss of vision.
Analysis of conjunctival biopsy can sometimes suggest allergy in patients with chronic conjunctivitis.
What are the complications of ocular allergy?
Complications of ocular allergy, aside from debilitating aggravation, are not common. Chronis rubbing of the eyes may eventually result in a change in its curvature, making it more like a cone than a sphere, a condition called keratoconus. Poor corneal health may make it more susceptible to infection.
When disease is severe, new blood vessels and scarring that occurs across the cornea can cause large decreases in vision, and may only be reparable by surgery.
What is the treatment for ocular allergy?
Avoidance of triggering allergens is the number one way of treating allergy. Other conservative measures are often successful in treating mild allergy, and include frequent use of lubricating eye drops, chilled if possible, and preferably without preservatives.
Cool compresses help relieve symptoms and may lessen inflammation.
Topical therapy with drops that fight both histamine and mast cells, such as Patanol, has become an important weapon against allergy, and can be used daily.
Topical corticosteroids are useful for controlling active inflammation, but all efforts to treat without dependence on steroids should be made to avoid other complications of these medications; a mild topical corticosteroid is sometimes necessary.
Oral anti-allergy medications can be used to treat seasonal allergies, along with the component driving eye symptoms.
It is also important to treat any coexisting conditions that may affect the surface of the eye. Immunomodulatory therapy with oral cyclosporine can also be used for severe and unresponsive cases of AKC with success.
Refraining from use of contact lenses, either temporarily or permanently, may be the only solution to those patients with GPC. Those with developing GPC can be counseled on limiting contact lens use so they do not develop complete intolerance of lenses.
Anyone with chronic or severe allergies should consult an allergist, who can perform diagnostic allergy testing, make recommendations to treat systemic allergy, and, if needed, provide regular injections to help limit reactions.
Corneal surgery can be attempted for those with scarring of central cornea, or in cases where chronic rubbing of the eyes has resulted in severe irregular astigmatism or keratoconus.
Our Physicians
All of our physicians have completed Fellowships in their specialty.
C. Stephen Foster, MD, FACS, FACR
Founder
Stephen D. Anesi, MD, FACS
Partner and Co-President
Peter Y. Chang, MD, FACS
Partner and Co-President
Peter L. Lou, MD
Associate
