Psoriasis and Eye Inflammation
By Peter Y. Chang, MD, FACS
August is Psoriasis Awareness month. Do you know that there is an association between psoriasis and uveitis and other types of inflammatory eye diseases?
Psoriasis is due to an overactive immune system resulting in an accelerated growth rate of skin cells. It is characterized by patches of red, scaly, and itchy skin on the elbows, knees, and scalp, though it can involve any part of the body. It is estimated that more than 3% of Americans are diagnosed with psoriasis. The disease affects both genders equally, and the average age of onset is between 15 and 35 years. There are multiple types of psoriasis depending on the clinical appearance and lesion distribution: plaque (most common), pustular, inverse, guttate, and erythrodermic (most severe and potentially life-threatening). Patients with psoriasis complain of red and irritated skin with silvery scales (figure 1), and some patients can have arthritis frequently involving the hand, foot, knee, and tendon insertion site. Psoriatic (and other inflammatory) arthritis is different from osteoarthritis in that it is worse in the morning or after a period of inactivity; tends to involve the whole fingers and toes and not just the knuckles (figure 2); and often asymmetric between the right and left sides of the body. In addition, patients with psoriatic arthritis may have characteristic changes on their finger and toe nails, such as nail separation from nail bed, pitting, and change in color that may be confused with a fungal infection (figure 3). The treatment of psoriasis typically consists of topical medications, but when the disease is severe, phototherapy and systemic immunomodulatory therapies such as methotrexate, cyclosporine, and various biologics may be needed.
Patients with severe psoriasis and/or psoriatic arthritis are more likely than the general population to develop eye inflammation. The link is perhaps not surprising, as an overactive immune system can attack more than one area of the body. Anterior uveitis (“iritis”) is by far the most common type of eye inflammation in psoriasis, but dry eye, conjunctivitis, episcleritis, and scleritis can all occur. It is important for psoriasis patients and their family to become familiarized with the symptoms and signs of uveitis, and not let a red and painful eye written off in the local emergency room or urgent care center simply as “pink eye.” A patient with anterior uveitis has significant eye pain, light sensitivity, floaters and, in more severe cases, loss of vision. On the other hand, pink eye (AKA viral conjunctivitis) is characterized by mucus discharge and swollen eyelids, but pain, light sensitivity, and vision loss are usually minimal.
At MERSI, we treat many patients with uveitis associated with psoriasis and psoriatic arthritis. The skin lesions of psoriasis typically precede the development of either joint or eye inflammation; however, it is not uncommon for us to discover psoriasis while examining the skin of patients during their initial valuation of uveitis, with subsequent dermatologic referral. When it comes to treatment, we advocate for a team approach in which we engage a patient’s dermatologist and rheumatologist in selecting the most effective systemic therapy that can bring forth inflammatory control in the skin, the joints, and the eye.
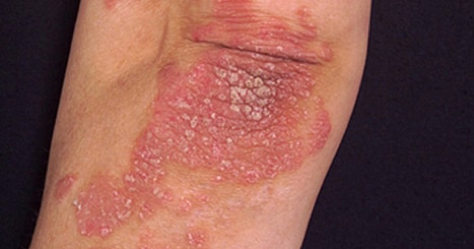
Figure 1. Typical appearance of psoriasis on the elbow (Image source: Mayo Foundation)
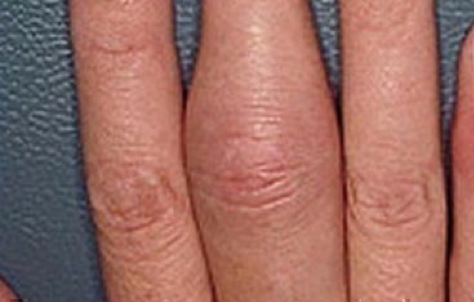
Figure 2. Psoriatic arthritis leading to swollen fingers, also called “sausage digits” (Image source: American Academy of Dermatology)

Figure 3. Nail psoriasis with nail pitting (Image source: American Academy of Dermatology)
